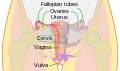
Uterus
| Uterus | |
|---|---|
 Diagram of human uterus and surrounding structures | |
| Details | |
| Precursor | Paramesonephric ducts |
| System | Reproductive system |
| Artery | Ovarian artery and uterine artery |
| Vein | Uterine veins |
| Lymph | Body and cervix to internal iliac lymph nodes, fundus to para-aortic lymph nodes, lumbar and superficial inguinal lymph nodes |
| Identifiers | |
| Latin | uterus |
| Greek | ὑστέρα (hystéra) |
| MeSH | D014599 |
| TA98 | A09.1.03.001 |
| TA2 | 3500 |
| FMA | 17558 |
| Anatomical terminology | |
The uterus (from Latin uterus, pl.: uteri or uteruses) or womb (/wuːm/) is the organ in the reproductive system of most female mammals, including humans, that accommodates the embryonic and fetal development of one or more fertilized eggs until birth.[1] The uterus is a hormone-responsive sex organ that contains glands in its lining that secrete uterine milk for embryonic nourishment. (The term uterus is also applied to analogous structures in some non-mammalian animals.)
In the human, the lower end of the uterus is a narrow part known as the isthmus that connects to the cervix, the anterior gateway leading to the vagina. The upper end, the body of the uterus, is connected to the fallopian tubes at the uterine horns; the rounded part, the fundus, is above the openings to the fallopian tubes. The connection of the uterine cavity with a fallopian tube is called the uterotubal junction. The fertilized egg is carried to the uterus along the fallopian tube. It will have divided on its journey to form a blastocyst that will implant itself into the lining of the uterus – the endometrium, where it will receive nutrients and develop into the embryo proper, and later fetus, for the duration of the pregnancy.
In the human embryo, the uterus develops from the paramesonephric ducts, which fuse into the single organ known as a simplex uterus. The uterus has different forms in many other animals and in some it exists as two separate uteri known as a duplex uterus.
In medicine and related professions, the term uterus is consistently used, while the Germanic-derived term womb is commonly used in everyday contexts. Events occurring within the uterus are described with the term in utero.
Structure
[edit]
In humans, the uterus is located within the pelvic region immediately behind and almost overlying the bladder, and in front of the sigmoid colon. The human uterus is pear-shaped and about 7.6 cm (3.0 in) long, 4.5 cm (1.8 in) broad (side to side), and 3.0 cm (1.2 in) thick.[2][3] A typical adult uterus weighs about 60 grams. The uterus can be divided anatomically into four regions: the fundus – the uppermost rounded portion of the uterus above the openings of the fallopian tubes,[4] the body, the cervix, and the cervical canal. The cervix protrudes into the vagina. The uterus is held in position within the pelvis by ligaments, which are part of the endopelvic fascia. These ligaments include the pubocervical ligaments, the cardinal ligaments, and the uterosacral ligaments. It is covered by a sheet-like fold of peritoneum, the broad ligament.[5]
Layers
[edit]| Location | Mean (mm) | Range (mm) |
|---|---|---|
| Anterior wall | 23 | 17 - 25 |
| Posterior wall | 21 | 15 - 25 |
| Fundus | 20 | 15 - 22 |
| Isthmus | 10 | 8 - 22 |

The uterus has three layers, which together form the uterine wall. From innermost to outermost, these layers are the endometrium, myometrium, and perimetrium.[7]
The endometrium is the inner epithelial layer, along with its mucous membrane, of the mammalian uterus. It has a basal layer and a functional layer; the functional layer thickens and then is shed during the menstrual cycle or estrous cycle. During pregnancy, the uterine glands and blood vessels in the endometrium further increase in size and number and form the decidua. Vascular spaces fuse and become interconnected, forming the placenta, which supplies oxygen and nutrition to the embryo and fetus.[8][9]
The myometrium of the uterus mostly consists of smooth muscle. The innermost layer of myometrium is known as the junctional zone, which becomes thickened in adenomyosis.[10]
The perimetrium is a serous layer of visceral peritoneum. It covers the outer surface of the uterus.[11]
Surrounding the uterus is a layer or band of fibrous and fatty connective tissue called the parametrium that connects the uterus to other tissues of the pelvis.
Commensal and mutualistic organisms are present in the uterus and form the uterine microbiome.[12][13][14][15]
Support
[edit]
The uterus is primarily supported by the pelvic diaphragm, perineal body, and urogenital diaphragm. Secondarily, it is supported by ligaments, including the peritoneal ligament and the broad ligament of uterus.[16]
Major ligaments
[edit]The uterus is held in place by several peritoneal ligaments, of which the following are the most important (there are two of each):
| Name | From | To |
|---|---|---|
| Uterosacral ligaments | Posterior cervix | Anterior face of sacrum |
| Cardinal ligaments | Side of the cervix | Ischial spines |
| Pubocervical ligaments[16] | Side of the cervix | Pubic symphysis |
Axis
[edit]Normally, the human uterus lies in anteversion and anteflexion. In most women, the long axis of the uterus is bent forward on the long axis of the vagina, against the urinary bladder. This position is referred to as anteversion of the uterus. Furthermore, the long axis of the body of the uterus is bent forward at the level of the internal os with the long axis of the cervix. This position is termed anteflexion of the uterus.[17] The uterus assumes an anteverted position in 50% of women, a retroverted position in 25% of women, and a midposed position in the remaining 25% of women.[2]
Position
[edit]
The uterus is located in the middle of the pelvic cavity, in the frontal plane (due to the broad ligament of the uterus). The fundus does not extend above the linea terminalis, while the vaginal part of the cervix does not extend below the interspinal line. The uterus is mobile and moves posteriorly under the pressure of a full bladder, or anteriorly under the pressure of a full rectum. If both are full, it moves upwards. Increased intra-abdominal pressure pushes it downwards. The mobility is conferred to it by a musculo-fibrous apparatus that consists of suspensory and sustentacular parts. Under normal circumstances, the suspensory part keeps the uterus in anteflexion and anteversion (in 90% of women) and keeps it "floating" in the pelvis. The meanings of these terms are described below:

| Distinction | More common | Less common |
|---|---|---|
| Position tipped | "Anteverted": Tipped forward | "Retroverted": Tipped backwards |
| Position of fundus | "Anteflexed": Fundus is pointing forward relative to the cervix | "Retroflexed": Fundus is pointing backward |

2. Anteversion with marked anteflexion
3. Anteversion with retrocession
4. Retroversion
5. Retroversion with retroflexion
The sustentacular part supports the pelvic organs and comprises the larger pelvic diaphragm in the back and the smaller urogenital diaphragm in the front.
The pathological changes of the position of the uterus are:
- retroversion/retroflexion, if it is fixed
- hyperanteflexion – tipped too forward; most commonly congenital, but may be caused by tumors
- anteposition, retroposition, lateroposition – the whole uterus is moved; caused by parametritis or tumors
- elevation, descensus, prolapse
- rotation (the whole uterus rotates around its longitudinal axis), torsion (only the body of the uterus rotates around)
- inversion
In cases where the uterus is "tipped", also known as retroverted uterus, the woman may have symptoms of pain during sexual intercourse, pelvic pain during menstruation, minor incontinence, urinary tract infections, fertility difficulties,[19] and difficulty using tampons. A pelvic examination by a doctor can determine if a uterus is tipped.[20]
Blood, lymph, and nerve supply
[edit]
The human uterus is supplied by arterial blood both from the uterine artery and the ovarian artery. Another anastomotic branch may also supply the uterus from anastomosis of these two arteries.
Afferent nerves supplying the uterus are T11 and T12. Sympathetic supply is from the hypogastric plexus and the ovarian plexus. Parasympathetic supply is from the S2, S3 and S4 nerves.
Development
[edit]
Bilateral Müllerian ducts form during early human fetal life. In males, anti-Müllerian hormone (AMH) secreted from the testes leads to the ducts' regression. In females, these ducts give rise to the fallopian tubes and the uterus. In humans, the lower segments of the two ducts fuse to form a single uterus; in cases of uterine malformations this fusion may be disturbed. The different uterine morphologies among the mammals are due to varying degrees of fusion of the Müllerian ducts.
Various congenital conditions of the uterus can develop in utero. Though uncommon, some of these are didelphic uterus, bicornate uterus and others.[21]
See also List of related male and female reproductive organs.
Function
[edit]
The primary reproductive function of the human uterus is to prepare for the implantation of a zygote, a fertilized ovum, and maintenance of pregnancy if implantation occurs.[22] Traveling along the fallopian tube on its way to the uterine cavity, the zygote divides mitotically to become a blastocyst, which ultimately attaches to the uterine wall and implants into the endometrium.[4] The placenta later develops to nourish the embryo, which grows through embryonic and fetal development until childbirth. During this process, the uterus grows to accommodate the growing fetus.[23] When normal labor begins, the uterus forcefully contracts as the cervix dilates, which results in delivery of the infant.[23]
In the absence of pregnancy, menstruation occurs.[22] The withdrawal of female sex hormones, estrogen and progesterone, which occurs in the absence of fertilization, triggers the shedding of the functional layer of the endometrium.[22] This layer is broken down, shed, and restored in anticipation of the next menstrual cycle.[22] The average bleeding duration during menses is 5-7 days after which the menstrual cycle begins again. [24]
Clinical significance
[edit]During pregnancy, the growth rate of the fetus can be assessed by measuring the fundal height.
Some pathological states include:

- Accumulation of fluids other than blood or of unknown constitution. One study came to the conclusion that postmenopausal women with endometrial fluid collection on gynecologic ultrasonography should undergo endometrial biopsy if the endometrial lining is thicker than 3 mm or if the endometrial fluid is echogenic. In cases of a lining 3 mm or less and clear endometrial fluid, endometrial biopsy was not regarded to be necessary, but endocervical curettage to rule out endocervical cancer was recommended.[25]
- Hematometra, which is accumulation of blood within the uterus.[26]
- Prolapse of the uterus
- Carcinoma of the cervix – malignant neoplasm
- Carcinoma of the uterus – malignant neoplasm
- Fibroids – benign neoplasms
- Adenomyosis – ectopic growth of endometrial tissue within the myometrium
- Endometritis, infection at the uterine cavity
- Pyometra – infection of the uterus, most commonly seen in dogs
- Asherman's syndrome, also known as intrauterine adhesions, occurs when the basal layer of the endometrium is damaged by instrumentation (e.g., D&C) or infection (e.g., endometrial tuberculosis) resulting in endometrial scarring followed by adhesion formation that partially or completely obliterates the uterine cavity
- Myometritis – inflammation of the muscular uterine wall.[27]
Malformations
[edit]
Uterine malformations are mainly congenital malformations, and include uterus didelphys, bicornuate uterus and septate uterus. Congenital absence of the uterus is known as Müllerian agenesis.
Surgery
[edit]A hysterectomy is the surgical removal of the uterus, which may be carried out for a number of reasons including the ridding of tumours both benign and malignant. A complete hysterectomy involves the removal of the body, fundus, and cervix of the uterus. A partial hysterectomy may just involve the removal of the uterine body while leaving the cervix intact. It is the most commonly performed gynecological surgical procedure.
Transplants
[edit]Uterus transplantations have been successfully carried out in a number of countries. The transplant is intended to be temporary – recipients will have to undergo a hysterectomy after one or two successful pregnancies. This is done to avoid the need to take immunosuppressive drugs for life with a consequent increased risk of infection.[28]
The procedure remains the last resort: it is as of 2023, a relatively new and somewhat experimental procedure, performed only by certain specialist surgeons in select centres, it is expensive and unlikely to be covered by insurance, and it involves risk of infection and organ rejection. Some ethics specialists consider the risks to a live donor too great, and some find the entire procedure ethically questionable, especially since the transplant is not a life-saving procedure.[29][30][31]
Other animals
[edit]Most animals that lay eggs, such as birds and reptiles, including most ovoviviparous species, have an oviduct instead of a uterus. However, recent research into the biology of the viviparous (not merely ovoviviparous) skink Trachylepis ivensi has revealed development of a very close analogue to eutherian mammalian placental development.[32]
In monotremes, mammals which lay eggs, namely the platypus and the echidnas, either the term uterus or oviduct is used to describe the same organ, but the egg does not develop a placenta within the mother and thus does not receive further nourishment after formation and fertilization.
Marsupials have two uteri, each of which connect to a lateral vagina and both use a third, middle "vagina", which functions as the birth canal.[33][34] Marsupial embryos form a choriovitelline placenta (which can be thought of as something between a monotreme egg and a "true" placenta), in which the egg's yolk sac supplies a large part of the embryo's nutrition but also attaches to the uterine wall and takes nutrients from the mother's bloodstream. However, bandicoots also have a rudimentary chorioallantoic placenta, similar to those of placental mammals.
The fetus usually develops fully in placental mammals and only partially in marsupials including kangaroos and opossums. In marsupials, the uterus forms as a duplex organ of two uteri. In monotremes such as the platypus, the uterus is duplex and rather than nurturing the embryo, secretes the shell around the egg. It is essentially identical with the shell gland of birds and reptiles, with which the uterus is homologous.[35]
In mammals, the four main forms of the uterus are: duplex, bipartite, bicornuate and simplex.[36]
- Duplex
- There are two wholly separate uteri, with one oviduct each. Found in marsupials (such as kangaroos, Tasmanian devils, opossums, etc.), rodents (such as mice, rats, and guinea pigs), and lagomorphs (rabbits and hares).
- Bipartite
- The two uteri are separate for most of their length, but share a single cervix. Found in ruminants (deer, moose, elk, etc.), hyraxes, cats, and horses.
- Bicornuate
- The upper parts of the uterus remain separate, but the lower parts are fused into a single structure. Found in dogs, pigs, elephants, whales, dolphins,[37] and tarsiers, and strepsirrhine primates among others.
- Simplex
- The entire uterus is fused into a single organ.[35] Found in higher primates (including humans and chimpanzees). Occasionally, some individual females (including humans) may have a bicornuate uterus, a uterine malformation where the two parts of the uterus fail to fuse completely during fetal development.
Two uteri usually form initially in a female and usually male fetus, and in placental mammals, they may partially or completely fuse into a single uterus depending on the species. In many species with two uteri, only one is functional. Humans and other higher primates such as chimpanzees, usually have a single completely fused uterus, although in some individuals, the uteri may not have completely fused.
Additional images
[edit]-
Schematic frontal view of female anatomy
-
Sectional plan of the gravid uterus in the third and fourth month
-
Fetus in utero, between fifth and sixth months.
-
Uterus
See also
[edit]- Artificial uterus
- Engineered uterus
- List of distinct cell types in the adult human body
- Menopause
- Social uterus
- Unicornuate uterus
- Uterus-like mass
- Gestational sac
References
[edit]- ^ Linzey, Donald W. (2020-08-04). Vertebrate Biology: Systematics, Taxonomy, Natural History, and Conservation. JHU Press. ISBN 978-1-4214-3733-0.
- ^ a b Manual of Obstetrics. (3rd ed.). Elsevier 2011. pp. 1–16. ISBN 9788131225561.
- ^ Donita, D'Amico (2015). Health & physical assessment in nursing. Barbarito, Colleen (3rd ed.). Boston: Pearson. p. 645. ISBN 9780133876406. OCLC 894626609.
- ^ a b "27.2 Anatomy and Physiology of the Female Reproductive System - Anatomy and Physiology | OpenStax". openstax.org. 25 April 2013. Retrieved 4 November 2022.
- ^ Gray's Anatomy for Students, 2nd edition
- ^ Nandita Palshetkar; Rishma Dhillon Pai; Hrishikesh D Pai (2012-09-30). Textbook of Hysteroscopy. JP Medical Ltd. pp. 135–. ISBN 978-93-5025-781-4.
- ^ Tortora, G; Derrickson, B (2011). Principles of anatomy & physiology (13th. ed.). Wiley. p. 1105. ISBN 9780470646083.
- ^ Blue Histology - Female Reproductive System Archived 2007-02-21 at the Wayback Machine. School of Anatomy and Human Biology — The University of Western Australia Accessed 20061228 20:35
- ^ Guyton AC, Hall JE, eds. (2006). "Chapter 81 Female Physiology Before Pregnancy and Female Hormones". Textbook of Medical Physiology (11th ed.). Elsevier Saunders. pp. 1018ff. ISBN 9780721602400.
- ^ "NCI Dictionary of Cancer Terms". National Cancer Institute. Archived from the original on 2017-12-26. Retrieved 2017-12-27.
- ^ Ross, Michael H.; Pawlina, Wojciech. Histology, a text and atlas (Sixth ed.). p. 848.
- ^ Franasiak, Jason M.; Scott, Richard T. (2015). "Reproductive tract microbiome in assisted reproductive technologies". Fertility and Sterility. 104 (6): 1364–1371. doi:10.1016/j.fertnstert.2015.10.012. ISSN 0015-0282. PMID 26597628.
- ^ Verstraelen, Hans; Vilchez-Vargas, Ramiro; Desimpel, Fabian; Jauregui, Ruy; Vankeirsbilck, Nele; Weyers, Steven; Verhelst, Rita; De Sutter, Petra; Pieper, Dietmar H.; Van De Wiele, Tom (2016). "Characterisation of the human uterine microbiome in non-pregnant women through deep sequencing of the V1-2 region of the 16S rRNA gene". PeerJ. 4: e1602. doi:10.7717/peerj.1602. ISSN 2167-8359. PMC 4730988. PMID 26823997.
- ^ Mor, Gil; Kwon, Ja-Young (2015). "Trophoblast-microbiome interaction: a new paradigm on immune regulation". American Journal of Obstetrics and Gynecology. 213 (4): S131–S137. doi:10.1016/j.ajog.2015.06.039. ISSN 0002-9378. PMC 6800181. PMID 26428492.
- ^ Payne, Matthew S.; Bayatibojakhi, Sara (2014). "Exploring Preterm Birth as a Polymicrobial Disease: An Overview of the Uterine Microbiome". Frontiers in Immunology. 5: 595. doi:10.3389/fimmu.2014.00595. ISSN 1664-3224. PMC 4245917. PMID 25505898.
- ^ a b The Pelvis University College Cork Archived from the original on 2008-02-27
- ^ Snell, Clinical Anatomy by regions, 8th edition
- ^ Bohannon, Cat (October 3, 2024). Eve: How the Female Body Drove 200 Million Years of Human Evolution. Penguin Random House. p. 76. ISBN 978-0385350549.
Female pelvic anatomy: it's a tight fit.
- ^ "Retroverted Uterus: What it is & How it Affects Pregnancy". www.womens-health.co.uk. Archived from the original on 2013-10-05.
- ^ Tipped Uterus:Tilted Uterus Archived 2011-02-24 at the Wayback Machine AmericanPregnancy.org. Accessed 25 March 2011
- ^ "Surgical Correction of Uterovaginal Anomalies | GLOWM". www.glowm.com. Archived from the original on 2017-12-28. Retrieved 2017-12-27.
- ^ a b c d Critchley, Hilary O. D.; Maybin, Jacqueline A.; Armstrong, Gregory M.; Williams, Alistair R. W. (2020-07-01). "Physiology of the Endometrium and Regulation of Menstruation". Physiological Reviews. 100 (3): 1149–1179. doi:10.1152/physrev.00031.2019. hdl:20.500.11820/36236a4e-a35e-4818-abe3-5d8b278c66f8. ISSN 0031-9333. PMID 32031903. S2CID 211063583.
- ^ a b Ameer, Muhammad Atif; Fagan, Sarah E.; Sosa-Stanley, Jessica N.; Peterson, Diana C. (2023), "Anatomy, Abdomen and Pelvis: Uterus", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 29262069, retrieved 2023-10-30
- ^ Thiyagarajan, Dhanalakshmi K.; Basit, Hajira; Jeanmonod, Rebecca (2023), "Physiology, Menstrual Cycle", StatPearls, Treasure Island (FL): StatPearls Publishing, PMID 29763196, retrieved 2023-10-30
- ^ Takacs P, De Santis T, Nicholas MC, Verma U, Strassberg R, Duthely L (November 2005). "Echogenic endometrial fluid collection in postmenopausal women is a significant risk factor for disease". J Ultrasound Med. 24 (11): 1477–81. doi:10.7863/jum.2005.24.11.1477. PMID 16239648. S2CID 20258522.
- ^ "Cervical Stenosis - Women's Health Issues - Merck Manuals Consumer Version". Merck Manuals Consumer Version. Archived from the original on 2018-11-08. Retrieved 2018-11-07.
- ^ "Myometritis - Medical Definition from MediLexicon". www.medilexicon.com. Archived from the original on 2016-12-29.
- ^ Ossola, Alexandra (18 February 2014). "Everything You Need To Know About Uterus Transplants". Popular Science. Retrieved 10 October 2014.
- ^ "Medical first: Baby born to woman who got new womb". Journal Star. 2006-2014 Gatehouse Media, Inc. 4 October 2014. Retrieved 4 October 2014.
- ^ "BBC News". 4 October 2014. Retrieved 5 October 2014.
- ^ "The Daily Telegraph". Telegraph.co.uk. 3 October 2014. Archived from the original on 4 October 2014. Retrieved 5 October 2014.
- ^ Blackburn, D. G.; Flemming, A. F. (2011). "Invasive implantation and intimate placental associations in a placentotrophic African lizard, Trachylepis ivensi (scincidae)". Journal of Morphology. 273 (2): 137–59. doi:10.1002/jmor.11011. PMID 21956253. S2CID 5191828.
- ^ Hugh Tyndale-Biscoe; Marilyn Renfree (30 January 1987). Reproductive Physiology of Marsupials. Cambridge University Press. ISBN 978-0-521-33792-2. Archived from the original on 10 April 2021. Retrieved 19 October 2020.
- ^ Ronald M. Nowak (7 April 1999). Walker's Mammals of the World. JHU Press. ISBN 978-0-8018-5789-8. Archived from the original on 10 April 2021. Retrieved 4 September 2017.
- ^ a b Romer, Alfred Sherwood; Parsons, Thomas S. (1977). The Vertebrate Body. Philadelphia, Pennsylvania: Holt-Saunders International. pp. 390–392. ISBN 0-03-910284-X.
- ^ Lewitus, Eric, and Christophe Soligo. "Life-history correlates of placental structure in eutherian evolution Archived 2017-09-06 at the Wayback Machine." Evolutionary Biology 38.3 (2011): 287-305.
- ^ Bernd Würsig; William F. Perrin; J.G.M. Thewissen (26 February 2009). Encyclopedia of Marine Mammals. Academic Press. ISBN 978-0-08-091993-5. Archived from the original on 10 April 2021. Retrieved 19 October 2020.
External links
[edit]- Anatomy photo:43:01-0102 at the SUNY Downstate Medical Center – "The Female Pelvis: Organs in the Female and male Pelvis in situ"
- Encyclopedia.com
- Uterus Anatomy
- Uterus Pregnancy