Clostridioides difficile
| Clostridioides difficile | |
|---|---|

| |
| C. difficile colonies on a blood agar plate | |
| |
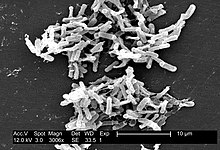
| Electron micrograph of the bacterium | |
| Scientific classification | |
| Domain: | Bacteria |
| Phylum: | Bacillota |
| Class: | Clostridia |
| Order: | Eubacteriales |
| Family: | Peptostreptococcaceae |
| Genus: | Clostridioides |
| Species: | C. difficile
|
| Binomial name | |
| Clostridioides difficile (Hall & O'Toole, 1935) Lawson & Rainey, 2016
| |
| Synonyms | |
Clostridioides difficile (syn. Clostridium difficile) is a bacterium known for causing serious diarrheal infections, and may also cause colon cancer.[4][5] It is known also as C. difficile, or C. diff (/siː dɪf/), and is a Gram-positive species of spore-forming bacteria.[6] Clostridioides spp. are anaerobic, motile bacteria, ubiquitous in nature and especially prevalent in soil. Its vegetative cells are rod-shaped, pleomorphic, and occur in pairs or short chains. Under the microscope, they appear as long, irregular (often drumstick- or spindle-shaped) cells with a bulge at their terminal ends (forms subterminal spores). Under Gram staining, C. difficile cells are Gram-positive and show optimum growth on blood agar at human body temperatures in the absence of oxygen. C. difficile is catalase- and superoxide dismutase-negative, and produces up to three types of toxins: enterotoxin A, cytotoxin B and Clostridioides difficile transferase.[7] Under stress conditions, the bacteria produce spores that are able to tolerate extreme conditions that the active bacteria cannot tolerate.[8]
Clostridioides difficile is an important emerging human pathogen; according to the CDC, in 2017 there were 223,900 cases in hospitalized patients and 12,800 deaths in the United States.[9] Although C. difficile is commonly known as a hospital and antibiotic associated pathogen, at most one third of infections can be traced to transmission from an infected person in hospitals,[10] and only a small number of antibiotics are directly associated with an elevated risk of developing a C. difficile infection (CDI), namely vancomycin, clindamycin, fluoroquinolones and cephalosporins.[11][12][13] The majority of infections are acquired outside of hospitals, and most antibiotics have similar elevated risk of infection on par with many non-antibiotic risk factors, such as using stool softeners and receiving an enema.[14]
Clostridioides difficile can also become established in the human colon without causing disease.[15] Although early estimates indicated that C. difficile was present in 2–5% of the adult population,[8] more recent research indicates colonization is closely associated with a history of unrelated diarrheal illnesses, such as food poisoning or laxative abuse.[16] Individuals with no history of gastrointestinal disturbances appear unlikely to become asymptomatic carriers. These carriers are thought to be a major reservoir of infection.[17]
Taxonomy
[edit]The species was transferred from the genus Clostridium to Clostridioides in 2016, thus giving it the binomial Clostridioides difficile.[18][19][20] This new name reflects the taxonomic differences between this species and members of the genus Clostridium, while maintaining the common name as C. diff.[19] As of 2018[update], the only other species in this new genus is Clostridioides mangenotii (formerly known as Clostridium mangenotii).[21]
Human pathogen
[edit]Pathogenic C. difficile strains produce multiple toxins.[22] The best-characterized are enterotoxin (C. difficile toxin A) and cytotoxin (C. difficile toxin B), both of which may produce diarrhea and inflammation in infected patients (C. difficile colitis), although their relative contributions have been debated. The diarrhea may range from a few days of intestinal fluid loss to life-threatening pseudomembranous colitis, which is associated with intense inflammation of the colon and formation of pseudomembranes on the intestinal mucosal surface.[8] This may progress to toxic megacolon, a severe form of colonic distention that can put a patient at risk for colon perforation, sepsis and shock. Toxins A and B are glucosyltransferases that target and inactivate the Rho family of GTPases. Toxin B (cytotoxin) induces actin depolymerization by a mechanism correlated with a decrease in the ADP-ribosylation of the low molecular mass GTP-binding Rho proteins.[23] There is also a binary toxin (AB toxin), but its role in disease is not fully understood.[24]
Additional virulence factors include an adhesion factor that mediates the binding to human colonic cells and a hyaluronidase.[25] The bacterium also produces the chemical para-cresol, which inhibits the growth of other microbes in its vicinity and allows it to outcompete normal human gut flora.[26]
Antimicrobial resistance
[edit]Antibiotic treatment of C. diff infections may be difficult, due both to antibiotic resistance and physiological factors of the bacterium (spore formation, protective effects of the pseudomembrane).[8] The emergence of a new, highly toxic strain of C. difficile, resistant to fluoroquinolone antibiotics, such as ciprofloxacin and levofloxacin, said to be causing geographically dispersed outbreaks in North America, was reported in 2005.[27] The U.S. Centers for Disease Control in Atlanta warned of the emergence of an epidemic strain with increased virulence, antibiotic resistance, or both.[28] Resistance to other antibiotics such as metronidazole, the first choice of antimicrobial drug when treating CDI, has been observed in up to 12% of clinical isolates, so as treatment with various antibiotics continues, more diverse and stronger resistances will continue to evolve in C. difficile populations, further complicating attempts at effective treatment.[29]
Disinfecting surfaces in hospitals may also be challenging as C. difficile spores resist many disinfectants,[30] including high concentrations of bleach.[31]
Transmission
[edit]
Clostridioides difficile is transmitted from person or animal to person by the fecal-oral route, shed in faeces. The organism forms heat-resistant aero-tolerant spores that are not killed by alcohol-based hand cleansers or routine surface cleaning, thus, these spores survive in clinical environments for long periods.[32] Any surface, device, or material (e.g., toilets, bathing tubs, and electronic rectal thermometers) that becomes contaminated with faeces may serve as a reservoir for the C. difficile spores, and C. difficile spores can live for long periods of time on surfaces.[33] Because of this, the bacterium may be cultured from almost any surface. Once spores are ingested, their acid resistance allows them to pass through the stomach unscathed. They germinate and multiply into vegetative cells in the colon upon exposure to bile acids. Consequently, the World Health Organization advocates the use of soap in addition to alcohol solutions to limit the spread of the spores.[34] Sporulation was shown to be significantly reduced after inactivation of C. diffiicile's DNA methyltransferase CamA,[35] raising the prospect of developing a drug that may inhibit this bacterium in a specific manner.
Susceptibility to colonization appears to be triggered by diarrheal illnesses, such as food poisoning, Crohn's disease or laxative abuse; people without a history of diarrheal illnesses who are exposed to C. difficile spores will not necessarily become carriers.[16] Once people are colonized by C. difficile, they remain carriers for year-long time scales, but the day-to-day abundance of C. difficile fluctuates considerably – fluctuating from being below the limit of detection to high levels of shedding from one day to the next. GI disturbances in carriers appear to trigger periods of increased shedding which may be an important factor for transmission.[citation needed]
Host range
[edit]Clostridioides difficile infects pigs, calves, and humans, and inhabits a natural reservoir of soil, faeces of domestic animals and humans, sewage, the human intestinal tract, and retail meat.[36]
A 2015 CDC study estimated that C. diff afflicted almost half a million Americans and caused 29,000 deaths in 2011. The study estimated that 40% of cases began in nursing homes or community health-care settings, while 24% occurred in hospitals.[37]
Clostridioides difficile is common in the human digestive system. However, it is a poor competitor, and is often outcompeted for nutrients by other bacteria in the digestive system. As a result, C. difficile is kept to a manageable number. If the sudden introduction of an antibiotic disrupts the microbiome, C. difficile may be able to grow as a result of many of its competitors being killed off. The incubation period is 5–10 days, with a range of 1 day to weeks following antibiotic treatment for antibiotic associated diarrhea. Additionally, carriage of C. difficile with high levels of toxins is common in young children, while disease is rare. The production of one or even both toxins is not always sufficient for producing symptoms.[38]
Signs and symptoms
[edit]Symptoms of C. difficile infection include diarrhea (at least three loose bowel movements a day), dehydration, abdominal pain that can be severe, loss of appetite, and nausea.[39]
Pathophysiology
[edit]C. difficile is transmitted through the oral-fecal route, and many reproduce through spores. The germination of these spores depends on the ability to sense primary bile acids in the liver, like taurocholate, which are sensed by the germinant receptor CspC. Secondary bile acids can inhibit these processes in the colon. Spores can grow and colonize the intestine by antibiotic-induced shifts in the host microbiota. C. difficile secretes mucolytic enzymes like CWp84 to degrade the colonic mucosa. These spores are also capable of adhering to colon cells. Additionally, C. difficile is a motile bacterium that can switch between both the motile and sessile phases, a process regulated by cyclic-di-GMP. On top of that, C. difficile is capable of forming biofilms and cell-to-cell signaling.[40] C. difficile is often transferred from other patients through the hands of healthcare workers or from the overall hospital environment and acquired from ingesting the pathogen. The spores resist the stomach acidity and germinate into their vegetative form in the small intestine. C. difficile can carry a broad spectrum of clinical manifestations, from being asymptomatic to severe colitis and death.[41] As such, C. difficile is the most prevalent U.S. healthcare infection, posing serious health risks and substantial care costs.[42]
Host immune response
[edit]The C. difficile secreted toxins A (TcdA) and B (TcdB), contain immunogenic antigens that are recognised by antibodies and T cells. However, the levels of anti-TcdA and -TcdB IgG antibodies have not been able to discriminate healthy individuals from patients with C. difficile infection, meaning they have limited clinical use.[43][44] Recent work has shown these toxins are also recognised by helper CD4+ T cells, predominantly by the Th17 helper cells, which are important in maintaining a healthy gut environment, although in patients with severe infection these cells are impaired.[45] Interestingly, individuals with severe C. difficile infection had significantly more toxin-specific T cells compared to those with mild infection, indicating T cells are playing a key role in fighting this infection. This immune response can further dysregulate microRNA expression.[46] This is further evidenced by the recovery of the toxin-specific Th17 cells and microRNA expression following Fecal microbiota transplant of patients with severe disease.[46][47] New findings show that the loss of the interleukin-10 corresponds to higher levels of interleukin-22, which has been found to be important in a host's response to a C.difficile infection. Thus, IL-10 deficiency can increase a host's defense against the pathogen. This could be of particular interest in future research for treatments. [48]
Diagnosis
[edit]A C. difficile infection is often suspected because of foul-smelling diarrhea, but this does not confirm if the patient has a CDI. To confirm a CDI, a cytotoxin assay detects the cell's toxin B (ToxB) cytotoxicity in the fecal eluate. The presence of C. difficile toxin is confirmed by the anti-toxin antibodies' neutralization of the cytotoxic effect. C. difficile strains can also be cultured before conducting a cytotoxin assay. These cultures detect the C. difficile strain that can produce toxins.[49] However, these enzyme immunoassays are more widely used due to their rapid turnaround, low cost, and simplicity. Additionally, they show lower sensitivity than toxigenic stool cultures. PCR assays have a shorter turnaround time and a higher sensitivity range than the toxigenic stool culture. Using a PCR-based assay helps avoid detection of asymptomatic patients. [41]
Treatment
[edit]Patients being treated with antibiotics when symptoms begin should stop taking them, if possible. This break in antibiotic therapy can sometimes lead to spontaneous resolution of symptoms. Patients who do not respond to the cessation of broad-spectrum antibiotics will need to be treated with antibiotics capable of killing C. difficile spores. Primary infections are typically treated with vancomycin, with a usual dosage of 125 mg every 6 hours.[50] The vancomycin regimen has replaced the traditional use of metronidazole due to its greater efficacy, safety profile, and lower recurrence rates. In patients who cannot tolerate vancomycin, fidaxomicin is an acceptable option with similar efficacy and even lower recurrence rates than vancomycin.[51] In cases of fulminant CDI, adjuvant therapy with parenteral metronidazole plus oral vancomycin or fidaxomicin is suggested.[52]
Approximately 15-30%[53] of patients who successfully complete therapy of primary infection with metronidazole or vancomycin will experience a relapse. About 40% of these patients will continue to have recurrent C. difficile infection. The first relapse of C. difficile is usually treated with the same antibiotic used to treat the primary infection. Any subsequent infections should not be treated with metronidazole. Occasionally, a standard 10-day course of oral vancomycin will not work. In these cases, a vancomycin taper is the preferred treatment. Patients take decreasing doses of vancomycin over a period of up to 3 months, depending on the severity of the infection.[39]
Each subsequent relapse of C. difficile tends to be more severe than previous infections. Long-term treatment with a vancomycin taper supplemented with probiotics, especially Saccharomyces boulardii, is associated with a higher rate of success.[54]
After three relapses, patients may be treated with oral fidaxomicin, a narrow-spectrum antibiotic. The usual dosage is 200 mg twice a day orally for 10 days. Fidaxomicin is considered to be superior to vancomycin for severe CDI.[55] The major downside of treatment with fidaxomicin is the cost of medication. A 10-day course may cost up to US$3500.[citation needed] When a patient is deteriorating or progressing to severe-complicated disease the addition of intravenous tigecycline merits considerations.[56][57] Patients with high risk of relapse may also benefit from the addition of the monoclonal antibody bezlotoxumab to the standard of care.[58]
Patients who do not respond to traditional antibiotic therapy may be eligible for a fecal microbiota transplant (FMT). Healthcare providers can transfer stool from a healthy person to the colon of a patient with recurrent CDI. This process is the most successful treatment for severe CDI with a cure rate around 93%. Fecal matter transplants have also been found to be an effective and safe treatment option for children and young adults.[59] Recurrence rates of CDI in patients treated with a FMT are generally low, around 19%, which makes it very effective at treating chronic CDI cases. However, in some cases, flares of inflammatory bowel disease are a possible side effect of the treatment.[60] The state of the host immune system is important when considering the success of microbiota-based treatments in clearing infection.[61] Long-term effects of FMT are unknown, as the procedure has only been FDA-approved for recurrent CDI since 2013 and relatively few procedures have been performed. If transplantation is not an option, removal of the infected part of the colon can cure CDI.[55][39]
In April 2023, the FDA approved the first oral microbiome therapeutic, VOWST for treatment of recurrent CDI.
The prediction of C. difficile recurrence has been of great interest, but there has been no consensus on significantly associated risk factors.[62]
Prevention
[edit]C. difficile infection is spread through the fecal-oral route through ingestion and acid-resistant spores. Appropriate hand hygiene of healthcare workers is vital to remove spores, which includes thoroughly washing one's hands with soap and warm water. Additionally, isolation of patients with acute diarrhea can prevent the spread of spores within the hospital. [63] Another way to prevent CDIs is wearing personal protective equipment when interacting with C. difficile patients. Furthermore, CDI transmission can be prevented by daily environmental sporicidal disinfection in patient rooms. Also, reducing the length of antibiotic therapy decreases the CDI rates in hospitals.[64]
Strains
[edit]In 2005, molecular analysis led to the identification of the C. difficile strain type characterized as group BI by restriction endonuclease analysis, as North American pulse-field-type NAP1 by pulsed-field gel electrophoresis and as ribotype 027; the differing terminology reflects the predominant techniques used for epidemiological typing. This strain is referred to as C. difficile BI/NAP1/027.[49]
As of 2016, the NAP1 strain has been replaced by novel strains in some areas of British Columbia. These novel strains include NAP2 and NAP4, and some strains that do not have a NAP designation. The frequency of these novel strains increased from 2008 to 2013 in one studied region, displacing the originally more common and recognizable NAP1 bacteria.[65]
Two strains, ribotypes RT078 and RT027, can live on low concentrations of the sugar trehalose; both strains became more common after trehalose was introduced as a food additive in the early 2000s, thus increasing dietary trehalose intake.[66]
Genome
[edit]| NCBI genome ID | 535 |
|---|---|
| Ploidy | haploid |
| Genome size | 4.3 Mb |
| Number of chromosomes | 1 |
| Year of completion | 2005 |
The first complete genome sequence of a C. difficile strain was published in 2005 by Sanger Institute in the UK. This was of the strain 630, a virulent and multiple drug-resistant strain isolated in Switzerland in 1982. Scientists at Sanger Institute have sequenced genomes of about 30 C. difficile isolates using next-generation sequencing technologies from 454 Life Sciences and Illumina.[67]
Researchers at McGill University in Montreal sequenced the genome of the highly virulent Quebec strain of C. difficile in 2005 using ultra-high throughput sequencing technology. The tests involved doing 400,000 DNA parallel-sequencing reactions of the bacterium's genome, which had been fragmented for sequencing. These sequences were assembled computationally to form a complete genome sequence.[27][68]
In 2012, scientists at University of Oxford sequenced C. difficile genomes from 486 cases arising over four years in Oxfordshire using next-generation sequencing technologies from Illumina.[69]
Epigenome
[edit]Clostridioides difficile has a highly diverse epigenome, with 17 high-quality methylation motifs reported so far, the majority pertaining to the 6mA type. Methylation at one of these motifs - CAAAAA, was shown to impact sporulation, a key step in C. difficile disease transmission, as well as cell length, biofilm formation, and host colonization.[35]
Bacteriophage
[edit]At least eight mainly temperate bacteriophages have been isolated from C. difficile, ranging in genome size from about 30 to about 60 kbp.[70] Both environmentally and clinically derived C. difficile strains carry a diverse and prevalent set of prophages.[70]
Etymology and pronunciation
[edit]References
[edit]- ^ Hall IC, O'toole E (1935). "Intestinal flora in new-born infants: with a description of a new pathogenic anaerobe, Bacillus difficilis". American Journal of Diseases of Children. 49 (2): 390–402. doi:10.1001/archpedi.1935.01970020105010.
- ^ Prévot AR (1938). "Études de systématique bactérienne. IV. Critique de la conception actuelle du genre Clostridium". Annales de l'Institut Pasteur. 61 (1): 84. Archived from the original on July 28, 2020. Retrieved December 15, 2018.
- ^ Page Species: Clostridioides difficile on "LPSN - List of Prokaryotic names with Standing in Nomenclature". Deutsche Sammlung von Mikroorganismen und Zellkulturen. Archived from the original on November 8, 2022. Retrieved November 8, 2022.
- ^ Drewes JL, Chen J, Markham NO, Knippel RJ, Domingue JC, Tam AJ, et al. (August 2022). "Human Colon Cancer-Derived Clostridioides difficile Strains Drive Colonic Tumorigenesis in Mice". Cancer Discovery. 12 (8): 1873–1885. doi:10.1158/2159-8290.CD-21-1273. PMC 9357196. PMID 35678528.
- ^ "Johns Hopkins Doctors Discover That a Common Infection May Cause Cancer". August 24, 2022. Archived from the original on May 26, 2023. Retrieved August 29, 2022.
- ^ Moreno MA, Furtner F, Rivara FP (June 2013). "Clostridium difficile: a cause of diarrhea in children". JAMA Pediatrics. 167 (6): 592. doi:10.1001/jamapediatrics.2013.2551. PMID 23733223.
- ^ Kordus SL, Thomas AK, Lacy DB (May 2022). "Clostridioides difficile toxins: mechanisms of action and antitoxin therapeutics". Nature Reviews. Microbiology. 20 (5): 285–298. doi:10.1038/s41579-021-00660-2. PMC 9018519. PMID 34837014.
- ^ a b c d Ryan KJ, Ray CG, eds. (2004). Sherris Medical Microbiology (4th ed.). McGraw Hill. pp. 322–4. ISBN 978-0-8385-8529-0.
- ^ "Clostridioides difficile Infection | HAI | CDC". www.cdc.gov. January 2, 2020. Archived from the original on March 8, 2020. Retrieved March 10, 2020.
- ^ Eyre DW, Cule ML, Wilson DJ, Griffiths D, Vaughan A, O'Connor L, et al. (September 2013). "Diverse sources of C. difficile infection identified on whole-genome sequencing". The New England Journal of Medicine. 369 (13): 1195–1205. doi:10.1056/NEJMoa1216064. PMC 3868928. PMID 24066741.
- ^ Guh AY, Adkins SH, Li Q, Bulens SN, Farley MM, Smith Z, et al. (October 1, 2017). "Risk Factors for Community-Associated Clostridium difficile Infection in Adults: A Case-Control Study". Open Forum Infectious Diseases. 4 (4): ofx171. doi:10.1093/ofid/ofx171. PMC 5903408. PMID 29732377.
- ^ Brown KA, Khanafer N, Daneman N, Fisman DN (May 2013). "Meta-analysis of antibiotics and the risk of community-associated Clostridium difficile infection". Antimicrobial Agents and Chemotherapy. 57 (5): 2326–2332. doi:10.1128/AAC.02176-12. PMC 3632900. PMID 23478961.
- ^ Rafey A, Jahan S, Farooq U, Akhtar F, Irshad M, Nizamuddin S, et al. (May 2023). "Antibiotics Associated With Clostridium difficile Infection". Cureus. 15 (5): e39029. doi:10.7759/cureus.39029. PMC 10266117. PMID 37323360.
- ^ McFarland LV, Surawicz CM, Stamm WE (September 1990). "Risk factors for Clostridium difficile carriage and C. difficile-associated diarrhea in a cohort of hospitalized patients". The Journal of Infectious Diseases. 162 (3): 678–684. doi:10.1093/infdis/162.3.678. PMID 2387993.
- ^ McFarland LV, Mulligan ME, Kwok RY, Stamm WE (January 1989). "Nosocomial acquisition of Clostridium difficile infection". The New England Journal of Medicine. 320 (4): 204–210. doi:10.1056/NEJM198901263200402. PMID 2911306.
- ^ a b VanInsberghe D, Elsherbini JA, Varian B, Poutahidis T, Erdman S, Polz MF (April 2020). "Diarrhoeal events can trigger long-term Clostridium difficile colonization with recurrent blooms". Nature Microbiology. 5 (4): 642–650. doi:10.1038/s41564-020-0668-2. PMID 32042128. S2CID 211074075.
- ^ Eyre DW, Griffiths D, Vaughan A, Golubchik T, Acharya M, O'Connor L, et al. (November 12, 2013). Chang YF (ed.). "Asymptomatic Clostridium difficile colonisation and onward transmission". PLOS ONE. 8 (11): e78445. Bibcode:2013PLoSO...878445E. doi:10.1371/journal.pone.0078445. PMC 3827041. PMID 24265690.
- ^ Oren A, Garrity GM (September 2017). "List of new names and new combinations previously effectively, but not validly, published". International Journal of Systematic and Evolutionary Microbiology. 67 (9): 3140–3143. doi:10.1099/ijsem.0.002278. PMC 5817221. PMID 28891789.
- ^ a b Lawson PA, Citron DM, Tyrrell KL, Finegold SM (August 2016). "Reclassification of Clostridium difficile as Clostridioides difficile (Hall and O'Toole 1935) Prévot 1938". Anaerobe. 40: 95–99. doi:10.1016/j.anaerobe.2016.06.008. PMID 27370902.
- ^ Zhu D, Sorg JA, Sun X (2018). "Clostridioides difficile Biology: Sporulation, Germination, and Corresponding Therapies for C. difficile Infection". Frontiers in Cellular and Infection Microbiology. 8: 29. doi:10.3389/fcimb.2018.00029. PMC 5809512. PMID 29473021.
- ^ Galperin MY, Brover V, Tolstoy I, Yutin N (December 2016). "Phylogenomic analysis of the family Peptostreptococcaceae (Clostridium cluster XI) and proposal for reclassification of Clostridium litorale (Fendrich et al. 1991) and Eubacterium acidaminophilum (Zindel et al. 1989) as Peptoclostridium litorale gen. nov. comb. nov. and Peptoclostridium acidaminophilum comb. nov". International Journal of Systematic and Evolutionary Microbiology. 66 (12): 5506–5513. doi:10.1099/ijsem.0.001548. PMC 5244501. PMID 27902180.
- ^ Di Bella S, Ascenzi P, Siarakas S, Petrosillo N, di Masi A (May 2016). "Clostridium difficile Toxins A and B: Insights into Pathogenic Properties and Extraintestinal Effects". Toxins. 8 (5): 134. doi:10.3390/toxins8050134. PMC 4885049. PMID 27153087.
- ^ Just I, Selzer J, von Eichel-Streiber C, Aktories K (March 1995). "The low molecular mass GTP-binding protein Rho is affected by toxin A from Clostridium difficile". The Journal of Clinical Investigation. 95 (3): 1026–1031. doi:10.1172/JCI117747. PMC 441436. PMID 7883950.
- ^ Barth H, Aktories K, Popoff MR, Stiles BG (September 2004). "Binary bacterial toxins: biochemistry, biology, and applications of common Clostridium and Bacillus proteins". Microbiology and Molecular Biology Reviews. 68 (3): 373–402, table of contents. doi:10.1128/MMBR.68.3.373-402.2004. PMC 515256. PMID 15353562.
- ^ [Medical Micriobiology, Fifth Edition, Patrick Murray, Elsevier Mosby, 2005, page 412]
- ^ "The chemical weapon that helps bacterium wreak havoc in the gut". Nature. 561 (7723): 288. September 14, 2018. Bibcode:2018Natur.561S.288.. doi:10.1038/d41586-018-06650-4. S2CID 52297840. Archived from the original on July 28, 2020. Retrieved October 8, 2018.
- ^ a b Loo VG, Poirier L, Miller MA, Oughton M, Libman MD, Michaud S, et al. (December 2005). "A predominantly clonal multi-institutional outbreak of Clostridium difficile-associated diarrhea with high morbidity and mortality". The New England Journal of Medicine. 353 (23): 2442–2449. doi:10.1056/NEJMoa051639. PMID 16322602. S2CID 14818750.
- ^ McDonald LC (August 2005). "Clostridium difficile: responding to a new threat from an old enemy". Infection Control and Hospital Epidemiology. 26 (8): 672–675. doi:10.1086/502600. PMID 16156321.
- ^ Banawas SS (February 21, 2018). "Clostridium difficile Infections: A Global Overview of Drug Sensitivity and Resistance Mechanisms". BioMed Research International. 2018: 8414257. doi:10.1155/2018/8414257. PMC 5841113. PMID 29682562.
- ^ Rashid T, Haghighi F, Hasan I, Bassères E, Alam MJ, Sharma SV, et al. (December 2019). "Activity of Hospital Disinfectants against Vegetative Cells and Spores of Clostridioides difficile Embedded in Biofilms". Antimicrobial Agents and Chemotherapy. 64 (1). doi:10.1128/AAC.01031-19. PMC 7187568. PMID 31611365.
- ^ "Bleach does not kill common superbug, study finds". BBC News. November 22, 2023. Archived from the original on November 22, 2023. Retrieved November 22, 2023.
- ^ Di Bella S, Sanson G, Monticelli J, Zerbato V, Principe L, Giuffrè M, et al. (February 29, 2024). Staley C (ed.). "Clostridioides difficile infection: history, epidemiology, risk factors, prevention, clinical manifestations, treatment, and future options". Clinical Microbiology Reviews. 37 (2). Mayuresh Abhyankar: e0013523. doi:10.1128/cmr.00135-23. ISSN 0893-8512. PMID 38421181. Archived from the original on March 4, 2024. Retrieved March 4, 2024.
- ^ "Clostridium difficile Infection Information for Patients". Health-care Associated Infections (HAI). U.S. Centers for Disease Control and Prevention. Archived from the original on March 30, 2017. Retrieved May 22, 2017.
- ^ "WHO Guidelines on Hand Hygiene in Health Care: a Summary" (PDF). World Health Organization. 2009. p. 31. Archived (PDF) from the original on May 9, 2020. Retrieved June 18, 2018.
- ^ a b Oliveira PH, Ribis JW, Garrett EM, Trzilova D, Kim A, Sekulovic O, et al. (January 2020). "Epigenomic characterization of Clostridioides difficile finds a conserved DNA methyltransferase that mediates sporulation and pathogenesis". Nature Microbiology. 5 (1): 166–180. doi:10.1038/s41564-019-0613-4. PMC 6925328. PMID 31768029.
- ^ Gould LH, Limbago B (September 2010). "Clostridium difficile in food and domestic animals: a new foodborne pathogen?". Clinical Infectious Diseases. 51 (5): 577–582. doi:10.1086/655692. PMID 20642351.
- ^ Belluck P (February 25, 2015). "Death Toll From C. Difficile Is Raised". The New York Times. Archived from the original on September 29, 2017. Retrieved February 25, 2015.
- ^ Murray P (2005). Medical Microbiology (Fifth ed.). Elsevier Mosby. p. 412.
- ^ a b c "Could you have deadly diarrhea (C. Diff)?". January 4, 2019. Archived from the original on March 30, 2017. Retrieved May 22, 2017.
- ^ Smits WK, Lyras D, Lacy DB, Wilcox MH, and Kuijper EJ (April 7, 2017). "Clostridium difficile infection". Nature Reviews Disease Primers. 2: 16020. doi:10.1038/nrdp.2016.20. PMC 5453186. PMID 27158839.
- ^ a b Lessa FC, Gould CV, McDonald LC (August 1, 2012). "Current Status of Clostridium difficile Infection Epidemiology". Clinical Infectious Diseases. 55 (Suppl 2): S65–S70. doi:10.1093/cid/cis319. PMC 3388017. PMID 22752867.
- ^ Cymbal M, Chatterjee A, Baggott B, Auron M (March 2024). "Management of Clostridioides difficile infection: Diagnosis, Treatment, and Future Perspectives". Am J Med. 137 (7): 571–576. doi:10.1016/j.amjmed.2024.03.024. PMID 38508330.
- ^ Monaghan TM, Negm OH, MacKenzie B, Hamed MR, Shone CC, Humphreys DP, et al. (July 2017). "High prevalence of subclass-specific binding and neutralizing antibodies against Clostridium difficile toxins in adult cystic fibrosis sera: possible mode of immunoprotection against symptomatic C. difficile infection". Clinical and Experimental Gastroenterology. 10: 169–175. doi:10.2147/CEG.S133939. PMC 5525456. PMID 28765714.
- ^ Wullt M, Norén T, Ljungh A, Åkerlund T (September 2012). "IgG antibody response to toxins A and B in patients with Clostridium difficile infection". Clinical and Vaccine Immunology. 19 (9): 1552–1554. doi:10.1128/CVI.00210-12. PMC 3428380. PMID 22787196.
- ^ Cook L, Rees WD, Wong MQ, Kwok WW, Levings MK, Steiner TS (March 2021). "Recurrent Clostridioides difficile Infection Is Associated With Impaired T Helper Type 17 Immunity to C difficile Toxin B". Gastroenterology. 160 (4): 1410–1413.e4. doi:10.1053/J.GASTRO.2020.11.043. PMID 33253683.
- ^ a b Bocchetti M, Ferraro MG, Melisi F, Grisolia P, Scrima M, Cossu AM, et al. (June 2023). "Overview of current detection methods and microRNA potential in Clostridioides difficile infection screening". World Journal of Gastroenterology. 29 (22): 3385–3399. doi:10.3748/wjg.v29.i22.3385. PMC 10303512. PMID 37389232.
- ^ Cook L, Rees WD, Wong MQ, Peters H, Levings MK, Steiner TS (May 2021). "Fecal Microbiota Transplantation for Recurrent Clostridioides difficile Infection Enhances Adaptive Immunity to C difficile Toxin B". Gastroenterology. 160 (6): 2155–2158.e4. doi:10.1053/J.GASTRO.2021.01.009. hdl:11343/289863. PMID 33444574. S2CID 231611318.
- ^ Cribas ES, Denny JE, Maslanka JR, Abt MC (April 16, 2021). "Loss of Interleukin-10 (IL-10) Signaling Promotes IL-22-Dependent Host Defenses against Acute Clostridioides difficile Infection". Infection and Immunity. 89 (5): e00730–20. doi:10.1128/IAI.00730-20. ISSN 1098-5522. PMC 8091099. PMID 33649048.
- ^ a b Rupnik M, Wilcox MH, Gerding DN (July 2009). "Clostridium difficile infection: new developments in epidemiology and pathogenesis". Nature Reviews. Microbiology. 7 (7): 526–536. doi:10.1038/nrmicro2164. PMID 19528959. S2CID 23376891.
- ^ McDonald LC, Gerding DN, Johnson S, Bakken JS, Carroll KC, Coffin SE, et al. (March 2018). "Clinical Practice Guidelines for Clostridium difficile Infection in Adults and Children: 2017 Update by the Infectious Diseases Society of America (IDSA) and Society for Healthcare Epidemiology of America (SHEA)". Clinical Infectious Diseases. 66 (7): e1–e48. doi:10.1093/cid/cix1085. PMC 6018983. PMID 29462280.
- ^ Mullane KM, Miller MA, Weiss K, Lentnek A, Golan Y, Sears PS, et al. (September 2011). "Efficacy of fidaxomicin versus vancomycin as therapy for Clostridium difficile infection in individuals taking concomitant antibiotics for other concurrent infections". Clinical Infectious Diseases. 53 (5): 440–447. doi:10.1093/cid/cir404. PMC 3156139. PMID 21844027.
- ^ Shane AL, Mody RK, Crump JA, Tarr PI, Steiner TS, Kotloff K, et al. (November 2017). "2017 Infectious Diseases Society of America Clinical Practice Guidelines for the Diagnosis and Management of Infectious Diarrhea". Clinical Infectious Diseases. 65 (12): e45–e80. doi:10.1093/cid/cix669. PMC 5850553. PMID 29053792.
- ^ Song JH, Kim YS (January 2019). "Recurrent Clostridium difficile Infection: Risk Factors, Treatment, and Prevention". Gut and Liver. 13 (1): 16–24. doi:10.5009/gnl18071. PMC 6346998. PMID 30400734.
- ^ "Treatment of Recurrent Clostridium difficile Colitis with Vancomycin and Saccharomyces boulardii" (PDF). The American Journal of Gastroenterology. Archived from the original (PDF) on August 9, 2017. Retrieved April 28, 2018.
- ^ a b Surawicz CM, Brandt LJ, Binion DG, Ananthakrishnan AN, Curry SR, Gilligan PH, et al. (April 2013). "Guidelines for diagnosis, treatment, and prevention of Clostridium difficile infections". The American Journal of Gastroenterology. 108 (4): 478–98, quiz 499. doi:10.1038/ajg.2013.4. PMID 23439232. S2CID 54629762.
- ^ van Prehn J, Reigadas E, Vogelzang EH, Bouza E, Hristea A, Guery B, et al. (December 2021). "European Society of Clinical Microbiology and Infectious Diseases: 2021 update on the treatment guidance document for Clostridioides difficile infection in adults" (PDF). Clinical Microbiology and Infection. 27 (Suppl 2): S1–S21. doi:10.1016/j.cmi.2021.09.038. PMID 34678515. S2CID 239473944.
- ^ Di Bella S, Nisii C, Petrosillo N (July 2015). "Is tigecycline a suitable option for Clostridium difficile infection? Evidence from the literature". International Journal of Antimicrobial Agents. 46 (1): 8–12. doi:10.1016/j.ijantimicag.2015.03.012. PMID 25982915.
- ^ Giacobbe DR, Dettori S, Di Bella S, Vena A, Granata G, Luzzati R, et al. (September 2020). "Bezlotoxumab for Preventing Recurrent Clostridioides difficile Infection: A Narrative Review from Pathophysiology to Clinical Studies". Infectious Diseases and Therapy. 9 (3): 481–494. doi:10.1007/s40121-020-00314-5. PMC 7452994. PMID 32632582.
- ^ AKAGAWA S, AKAGAWA Y, YAMANOUCHI S, KIMATA T, TSUJI S, KANEKO K (August 25, 2020). "Development of the gut microbiota and dysbiosis in children". Bioscience of Microbiota, Food and Health. 40 (1): 12–18. doi:10.12938/bmfh.2020-034. PMC 7817514. PMID 33520564.
- ^ Chen T, Zhou Q, Zhang D, Jiang F, Wu J, Zhou JY, et al. (May 2018). "Effect of Faecal Microbiota Transplantation for Treatment of Clostridium difficile Infection in Patients With Inflammatory Bowel Disease: A Systematic Review and Meta-Analysis of Cohort Studies". Journal of Crohn's & Colitis. 12 (6): 710–717. doi:10.1093/ecco-jcc/jjy031. PMID 29528385. S2CID 3841585.
- ^ Littmann ER, Lee JJ, Denny JE, Alam Z, Maslanka JR, Zarin I, et al. (February 2, 2021). "Host immunity modulates the efficacy of microbiota transplantation for treatment of Clostridioides difficile infection". Nature Communications. 12 (1): 755. Bibcode:2021NatCo..12..755L. doi:10.1038/s41467-020-20793-x. ISSN 2041-1723. PMC 7854624. PMID 33531483.
- ^ Stewart DB, Berg A, Hegarty J (January 2013). "Predicting Recurrence of C. difficile Colitis Using Bacterial Virulence Factors: Binary Toxin Is the Key". Journal of Gastrointestinal Surgery. 17 (1): 118–125. doi:10.1007/s11605-012-2056-6. PMID 23086451. Archived from the original on March 21, 2024. Retrieved March 20, 2024.
- ^ Burke KE, Lamont JT (January 29, 2014). "Clostridium difficile Infection: A Worldwide Disease". Gut Liver. 8 (1): 1–6. doi:10.5009/gnl.2014.8.1.1. PMC 3916678. PMID 24516694.
- ^ Tschudin-Sutter S, Kuijper EJ, Durovic A, Vehreschild MJ, Barbut F, Eckert C, et al. (October 2018). "Guidance document for prevention of Clostridium difficile infection in acute healthcare settings". Clinical Microbiology and Infection. 24 (10): 1051–1054. doi:10.1016/j.cmi.2018.02.020. PMID 29505879.
- ^ Jassem AN, Prystajecky N, Marra F, Kibsey P, Tan K, Umlandt P, et al. (March 29, 2016). "Characterization of Clostridium difficile Strains in British Columbia, Canada: A Shift from NAP1 Majority (2008) to Novel Strain Types (2013) in One Region". The Canadian Journal of Infectious Diseases & Medical Microbiology. 2016: 8207418. doi:10.1155/2016/8207418. PMC 4904575. PMID 27366181.
- ^ Collins J, Robinson C, Danhof H, Knetsch CW, van Leeuwen HC, Lawley TD, et al. (January 2018). "Dietary trehalose enhances virulence of epidemic Clostridium difficile". Nature. 553 (7688): 291–294. Bibcode:2018Natur.553..291C. doi:10.1038/nature25178. PMC 5984069. PMID 29310122.
- ^ He M, Sebaihia M, Lawley TD, Stabler RA, Dawson LF, Martin MJ, et al. (April 2010). "Evolutionary dynamics of Clostridium difficile over short and long time scales". Proceedings of the National Academy of Sciences of the United States of America. 107 (16): 7527–7532. Bibcode:2010PNAS..107.7527H. doi:10.1073/pnas.0914322107. PMC 2867753. PMID 20368420.
- ^ Scientists map C. difficile strain Archived May 22, 2022, at the Wayback Machine – Institute of Public Affairs, Montreal
- ^ Didelot X, Eyre DW, Cule M, Ip CL, Ansari MA, Griffiths D, et al. (December 2012). "Microevolutionary analysis of Clostridium difficile genomes to investigate transmission". Genome Biology. 13 (12): R118. doi:10.1186/gb-2012-13-12-r118. PMC 4056369. PMID 23259504.
- ^ a b Hargreaves KR, Clokie MR (2014). "Clostridium difficile phages: still difficult?". Frontiers in Microbiology. 5: 184. doi:10.3389/fmicb.2014.00184. PMC 4009436. PMID 24808893.
External links
[edit]- Pathogen Safety Data Sheets: Infectious Substances – Clostridium Difficile[permanent dead link], Public Health Agency, Canada, September 10, 2014.
- Type strain of Clostridium difficile, BacDive - the Bacterial Diversity Metadatabase.
